The University of Michigan ER is like nothing I’ve ever experienced. It feels enormous—hundreds of rooms, providers, nurses, techs—all moving with purpose. From the moment you step inside, everything runs like a well-oiled machine: labs, imaging, scans, consults. You can’t help but feel that you’re in the best possible hands.
While in the ER, I had viral panels drawn and repeat lab work, all of which came back normal. The team decided to admit me to the oncology floor, but due to bed shortages I was boarded in the ER for nearly 24 hours. When I was finally transferred upstairs, I felt a strange mix of emotions—relief and even joy at first, followed quickly by dread. This was the cancer floor. I could hear people crying out in pain. Deep, rattling coughs echoed down the hallway. It was a stark reminder that my future may not be as bright as I’d hoped.
I had a lovely roommate who was on hospice. I didn’t know much about her story, but just knowing she was likely out of options was deeply upsetting.
I stayed in the hospital for three days. Repeat scans showed a “mixed response” to my current chemotherapy—some lesions had shrunk, some had grown, and others remained stable. All viral testing was negative. The team was preparing to discharge me when they began asking more detailed questions about my headaches. The only remaining test was a lumbar puncture. I reluctantly agreed, knowing that if I went home and developed another severe headache, I’d always wonder if I’d made the wrong decision.
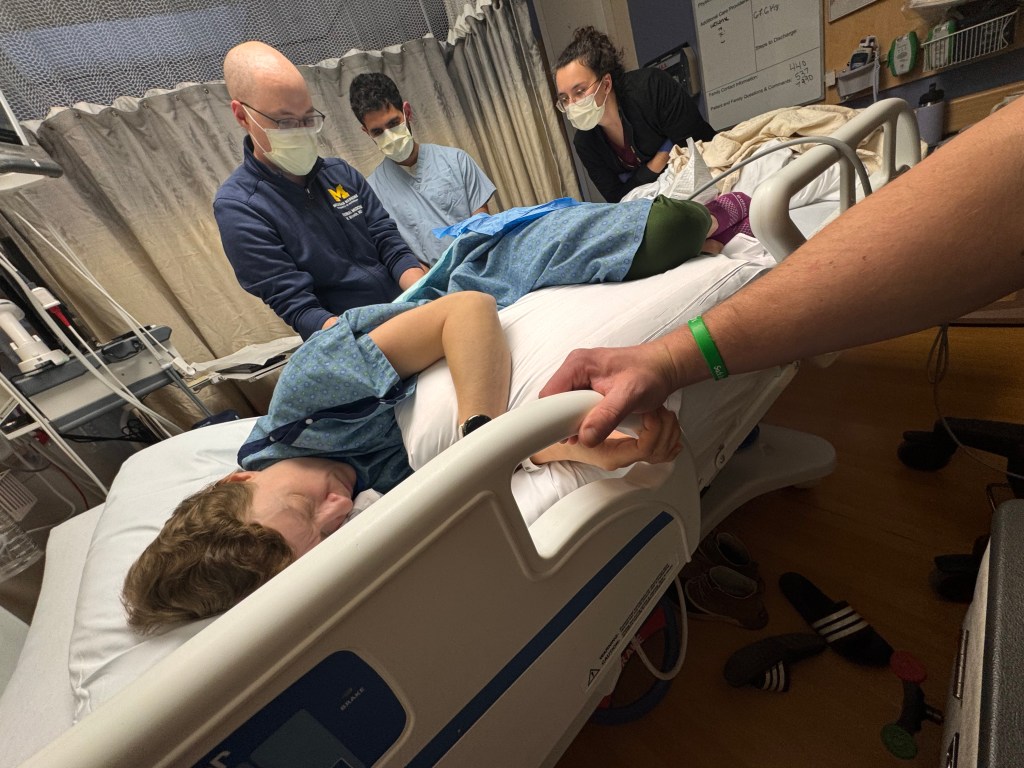
As unenthusiastic as I was about having an LP, it was oddly one of those procedures I’d always wanted to experience firsthand—purely from a medical curiosity standpoint. I found myself excited for whoever would get to perform it. A PA, an attending, and a resident were present. The attending carefully walked the resident through each step. Once the dura mater was punctured and cerebrospinal fluid began to flow, I gathered the courage to ask the resident how many LPs he had performed. I believe I was his third. Honestly, he did a wonderful job—it was far less painful than I had anticipated.
After the CSF was collected, the tubes were placed in a bag. As the attending walked away to wash his hands, his body brushed against the bag and it fell to the floor. I will never forget the look on Nick’s face. He stared directly into the attending’s soul, clearly convinced every tube had shattered. Without missing a beat, the attending calmly said, “No big deal—they’re plastic,” cool as a cucumber.
I stayed one additional night and was discharged the following day. I did feel a bit frustrated that neither my ACC team nor oncology formally saw me during my hospitalization. By that point, my fevers had resolved, but I still had persistent achiness, headaches, and night sweats.
A few days later, I followed up with my ACC specialist. He believes my fevers were most likely medication-related. I shared my own theory—that the combination of a recent COVID infection and immunotherapy may have triggered some sort of cytokine overresponse. He agreed it was possible, but there’s really no way to know for certain. He explained again that my tumor showed a mixed response and referred me to U of M oncology in case any unusual symptoms arise in the future. I was reassured to learn that they use a single oncologist for all ACC patients, meaning much deeper experience with the medications I’m on. He also planned to present my case at tumor board the following week.
I asked his thoughts on the ADCT-701 clinical trial at the NIH and was surprised to learn he wasn’t very familiar with it.
I was given the green light to resume my medications. I received my Keytruda infusion a few hours later and restarted cabozantinib the next day. Not long after, my symptoms finally resolved. I’m not sure if enough time had simply passed—or if restarting treatment somehow kicked my immune system back into gear—but either way, it felt like turning a corner.
Leave a comment